Published in Duluthian March/April 2018
St. Luke's Advanced Stroke Treatment
When it comes to treating a stroke, time is critical. Medical professionals
refer to this as “time is brain,” meaning the more time it
takes to get the patient appropriate care, the more brain cells are lost.
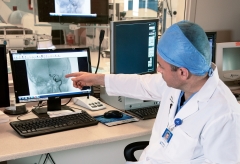
Dr. Morgan Althoen, an Interventional Radiologist at St. Luke’s Hospital,
said, “We know that for about every 30 minutes the clot stays in
the brain, the patient's chance of getting a really good functional
outcome decreases by 12 percent.”
According to recent American Heart Association (AHA) statistics, stroke
is the second-leading cause of death in the world and a leading cause
of adult disability. It kills about 133,000 Americans every year, and
occurs in the U.S. about once every 40 seconds.
Acute ischemic stroke is the most common type, caused by a blood clot that
reduces or stops blood flow to a portion of the brain. One of the treatment
options for some acute ischemic stroke patients is a procedure called
stroke thrombectomy.
Recent changes in the AHA guidelines now recommend that more people should
be considered for thrombectomies. The clot retrieval procedure requires
a physician to thread a catheter through the femoral artery and then to
the brain, using a clot-grabbing device within it to reach and remove the clot.
Recognized for their stroke care by the AHA and by the American Stroke
Association (ASA), St. Luke’s is the only hospital in the region
to offer the option of stroke thrombectomies. Their highly trained staff
and state-of-the-art hybrid operating room, save time and brain for their patients.
Until relatively recently, area patients could only receive stroke thrombectomies
in the Twin Cities. The travel time to the Twin Cities for patients was
not conducive to them getting care as timely as possible.
Stan Sadenwasser, St. Luke’s Cardiovascular Services Coordinator,
said, “We’re very, very fortunate to be able to provide stroke
thrombectomies which have a success rate of 70 to 75 percent for qualifying
patients.”
Dr. Althoen said, “Since people often don’t have any symptoms
or pain with a stroke, patients who get them in their sleep might not
even know it until several hours afterwards.”
“While it doesn’t cure everybody, the procedure gives some
patients the best chance for recovery. Time is of the essence to get the
patient to the hospital, get the stroke diagnosed and then followup with
the best plan for each patient,” Dr. Althoen added.
The thrombectomy procedure was life-saving for Beverly Talonen, a Grand
Rapids mother and grandmother. She described a frightening night that
happened this past New Year’s Eve after she had gone to bed and
fallen asleep. “I woke up at 3 a.m. to go to the bathroom and I
couldn’t think of how to get out of bed,” she said.
When Beverly woke her husband to tell him, he quickly came around to her
side of the bed to help her up. As she tried to stand up and to put weight
on her left leg, she crumpled and fell to the floor.
“I told my husband, I think I am having a stroke. Call 911,”
Beverly related. After getting to the area hospital by ambulance and having
an MRI and a CT scan, the doctors determined she should be flown to St.
Luke’s in Duluth for treatment for what had been a stroke.
While Beverly remembers few details of the flight to Duluth or of the rest
of that night, Dr. Althoen and his team had performed a successful thrombectomy
and had removed the clot from her brain.
After the procedure and her ten days of recovery and rehabilitation at
St. Luke’s, she was able to go back home. “I feel really great.
I am still doing physical therapy, and I am working on getting my strength
back,” she said.
Beverly noted that if she would have had to be flown to a Minneapolis hospital
for treatment instead of to St. Luke’s in Duluth, she probably would
not have survived or would have come out of this with possibly serious
impairments.
She said, “I have always been a positive person. I came through cancer
six years ago. Both the cancer and the stroke reminded me that you need
to enjoy every day you’ve got spending time with your loved ones.”
NBC Nightly News reported in their January 24, 2018 broadcast that with
the new stroke guidelines “more people could be eligible for life-saving
clot removal and treatments, expanding the ‘golden window’
when doctors can minimize or prevent permanent damage from six to 24 hours.”
The news report quoted Dr. William J. Powers, the guideline writing group
chair and professor of neurology at the University of North Carolina in
Chapel Hill, North Carolina. “The expanded time window for mechanical
thrombectomy for appropriate patients will allow us to help more patients
lower their risk of disability from stroke. That’s a big deal,” he said.
Dr. Althoen added, “It is very satisfying for St. Luke’s to
be the regional center for this procedure.”
Sidebar
The American Heart Association encourages everyone to learn how to recognize
the warning signs of strokes. Their F.A.S.T stroke campaign makes the
sudden signs and symptoms easy to remember:
Face Drooping - Does one side of the face droop or is it numb? Ask the person
to smile and check if their smile is lopsided or uneven.
Arm Weakness - Is one arm numb or weak? Ask the person to raise their arms
to check if one side drifts downward or have them squeeze your hands to
see if each side has equal strength.
Speech Difficulty - Is the person hard to understand, slurring their words
or unable to speak? Ask them to repeat a simple phrase.
Time to Call 911 - If you can see any of these signs, you should call 9-1-1
for immediate medical attention and get that person to a hospital immediately
- even if the symptoms go away. Tell medical staff they are showing signs
of a stroke and what time you began to see the signs.
BELOW: Dr. Morgan Althoen, St. Luke's Interventional Radiologist